
Regular dental care is important to your overall health. You may purchase coverage in either DeltaCare USA DHMO High/Medium options or MetLife PPO (explained below).
You may choose to purchase dental coverage within 60 days of the date when first eligible. Once you enroll, you may not change dental coverage until the next open enrollment period (explained next).
Pensioners who did not enroll in dental coverage when first eligible may only enroll during the annual open enrollment period October 1 – November 30, 2025 for coverage that begins the following January 1. Download a Dental Enrollment Form or get a copy from the Fund Office or your local union during the open enrollment period. Dental coverage begins January 1 following the date your properly completed form is timely received by the Fund Office.
Both dental options—DeltaCare USA DHMO High or Medium and MetLife PPO—are listed on the Dental Enrollment Form. To enroll, you must select one of these two options. You may also choose to purchase DeltaCare USA DHMO or MetLife PPO coverage for your covered spouse or domestic partner under the same dental option as you.
Once complete, email, fax or mail a your Dental Enrollment Form to the Fund Office.
Note: If you elect DeltaCare USA DHMO, remember to select a network dentist near you and list the six-digit facility code on the Dental Enrollment Form. If left blank, DeltaCare USA will automatically assign you to the closest contracted provider based on your home zip code. You may change your dentist by contacting DeltaCare USA (DHMO) at any time.
You may request to terminate coverage at any time. If so, you may not re-enroll until the next open enrollment period.
Eligible participants may purchase coverage in DeltaCare USA (DHMO) or MetLife PPO:
DeltaCare USA (DHMO):
The High Option offers greater benefits for a higher monthly premium..
Visit this link for a summary.
The Medium Option offers lesser benefits for a lower monthly premium.
Visit this link for a summary.
Neither a dental deductible nor benefit maximum apply to either option.
For more details about your benefits, contact DeltaCare USA directly at (800) 422-4234 or www1.deltadentalins.com.
MetLife PPO:
Lets you visit any licensed dentist, but you’ll save the most by visiting a MetLife PPO contracted dentist.
Visit this link for a summary.
For more details about your benefits, contact MetLife PPO directly at (800) 942-0854 or metlife.com/mybenefits.
Monthly premiums for the DeltaCare USA DHMO and MetLife PPO options are shown in this chart. Keep in mind that premium amounts may change.
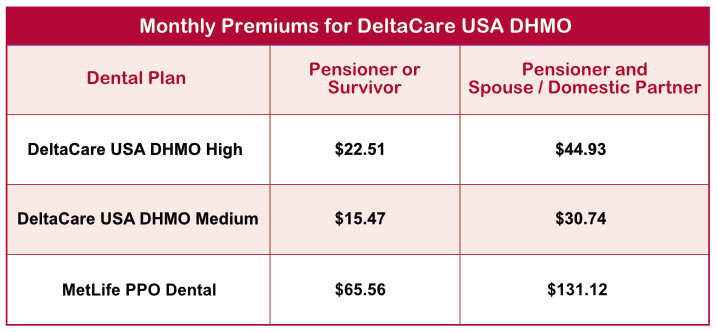
Note: This amount is in addition to the monthly premium for your medical coverage.
Dental premiums must be deducted from your Southern California Pipe Trades Retirement Fund pension benefit, if any. If you are not receiving a pension benefit (or if the pension benefit is not enough to cover the premiums), your premiums must be automatically deducted from a bank account. Contact the Fund Office for details.
Note: DeltaCare USA DHMO and MetLife PPO premiums will not be accepted by check, money order, cash or any other method.
TIP: Visit www1.deltadentalins.com or metlife.com/mybenefits to register or log in to your account to verify your benefits, access your digital ID card, change your assigned dentist and more.
Under either the High or Medium dental option, DeltaCare USA (DHMO) requires that all services and referrals be provided by your assigned DeltaCare USA network dentist. Benefits are only paid if services are performed by your assigned network dentist.
Both DeltaCare USA options are DHMOs. Before enrolling, check that the DeltaCare USA DHMO network operates where you live. Some areas may not have as many network dentists.
TIP: Remember to use your assigned DeltaCare USA dentist. If you want to choose a specific primary care dentist, list the 6-digit facility code on your Dental Enrollment Form. Remember, benefits are not paid if services are performed by non-network dental providers.
You can find DHMO dentists at www1.deltadentalins.com. Download their app to view coverage details, schedule or change appointments, access a digital ID card and estimate costs.
Click here for Frequently Asked Questions about dental coverage.
